Ultrasound Therapy for Pain: How Sound Waves Heal at the Cellular Level
Ultrasound Therapy for Pain: How Sound Waves Heal at the Cellular Level
When most people hear "ultrasound," they think of pregnancy imaging or a diagnostic scan. But therapeutic ultrasound — a technology that's been refined over decades — does something far more active than simply picture your insides. It sends precisely calibrated sound waves into your tissues, triggering a cascade of biological responses that reduce pain, accelerate healing, and restore cellular function.
If you're dealing with chronic pain, recovering from an injury, or simply curious about the intersection of physics and biology, understanding how ultrasound therapy works at the cellular level can change how you think about healing itself.
What Is Therapeutic Ultrasound?
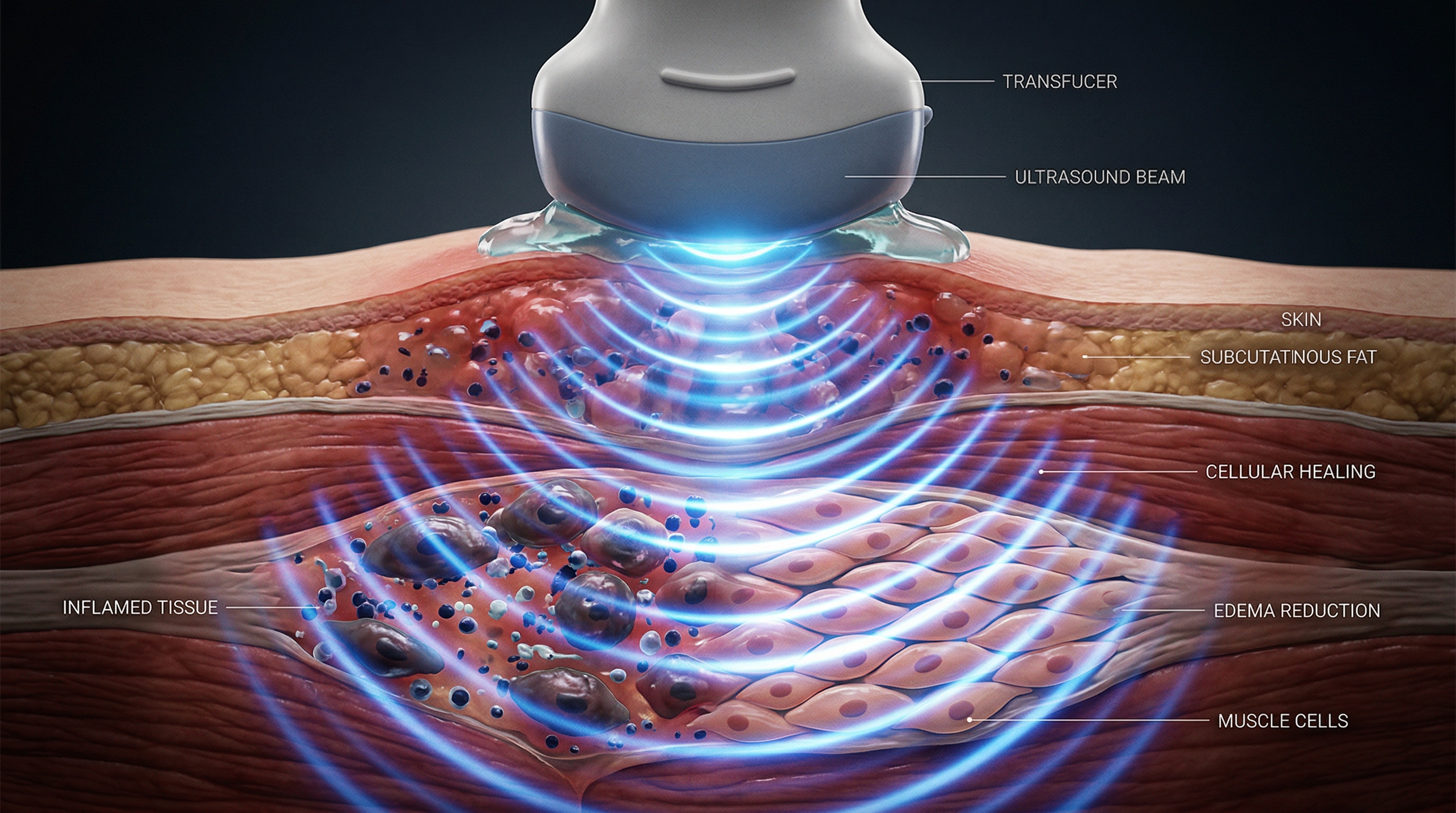
Therapeutic ultrasound uses high-frequency sound waves — typically between 0.8 and 3 MHz — delivered through a transducer probe applied to the skin. These sound waves travel through soft tissue and interact with cells in ways that are both mechanical and thermal. Unlike diagnostic ultrasound, which passively captures images, therapeutic ultrasound actively modulates tissue biology.
The treatment comes in two primary modes:
- Continuous mode — delivers a constant stream of acoustic energy, primarily generating heat in deep tissues
- Pulsed mode — delivers energy in rhythmic bursts, emphasizing non-thermal cellular effects while minimizing heat buildup
Both modes have distinct clinical applications, and choosing between them depends on whether the goal is pain relief through thermal relaxation or tissue repair through cellular stimulation.
The Two Mechanisms: Thermal and Non-Thermal Effects
Thermal Effects: Deep Tissue Warming
When ultrasound waves pass through tissue, their energy is absorbed — especially by collagen-rich structures like tendons, ligaments, and joint capsules. This absorption creates molecular friction, raising tissue temperature to between 40°C and 45°C. This isn't superficial warming; it penetrates several centimeters deep.
The therapeutic consequences of this deep heating include:
- Increased blood flow through vasodilation, delivering more oxygen and nutrients to damaged tissue
- Reduced muscle spasm as heated muscle fibers relax and become more pliable
- Pain gate modulation — heat stimulates sensory receptors that can override pain signal transmission
- Increased collagen extensibility, making stretching and mobilization more effective
Non-Thermal Effects: The Cellular Conversation
This is where ultrasound therapy becomes genuinely fascinating. Even at intensities too low to generate meaningful heat, pulsed ultrasound triggers powerful biological responses through three primary mechanisms:
Stable cavitation. Microscopic gas bubbles present in tissue fluids oscillate in response to the acoustic pressure waves. This oscillation alters cell membrane permeability — not destructively, but in a controlled way that increases ion transport (particularly sodium and calcium) and enhances the diffusion of nutrients and signaling molecules across cell membranes.
Acoustic streaming. The sound waves generate tiny, directional fluid currents along cell membranes. These micro-currents accelerate the transport of waste products away from cells while drawing fresh nutrients closer — essentially creating a microscopic irrigation system at the tissue level.
Mechanotransduction. Perhaps the most elegant mechanism. The mechanical force of sound waves is converted into biochemical signals when cells sense the physical stress through integrins (membrane receptors) and ion channels. This triggers intracellular signaling cascades — particularly the MAPK/ERK pathways — that regulate cell proliferation, differentiation, and migration.
Ultrasound doesn't just warm tissue. It speaks to cells in a mechanical language they're evolved to interpret — activating repair programs that would otherwise remain dormant.
How Ultrasound Heals at the Cellular Level
Fibroblast Activation
Fibroblasts are the construction workers of tissue repair. They synthesize collagen, build the extracellular matrix, and physically migrate to wound sites. Ultrasound significantly enhances fibroblast activity — increasing their mobility, accelerating collagen production, and improving the structural organization of newly deposited tissue. This is critical for tendon and ligament repair, where collagen alignment determines functional recovery.
Stem Cell Recruitment
Emerging research shows that low-intensity pulsed ultrasound (LIPUS) activates mesenchymal stem cells — promoting their adhesion, migration, and differentiation into the specific cell types needed for repair. It also upregulates growth factors like VEGF (vascular endothelial growth factor) and TGF-β (transforming growth factor beta), which orchestrate the entire healing cascade from inflammation through remodeling.
Anti-Inflammatory Signaling
Ultrasound modulates the inflammatory environment by downregulating pro-inflammatory cytokines while promoting anti-inflammatory mediators. This doesn't suppress the immune response — it helps resolve inflammation more efficiently, reducing the chronic low-grade inflammation that perpetuates pain conditions.
Osteoblast and Chondrocyte Stimulation
For bone healing, LIPUS has earned FDA clearance for fracture treatment. Clinical evidence shows it accelerates bone healing by approximately 38% compared to standard care. The mechanism involves stimulating osteoblast proliferation and differentiation, as well as enhancing the production of bone matrix proteins.
The Vagus Nerve Connection
One of the more intriguing applications of therapeutic ultrasound involves the vagus nerve — the body's primary parasympathetic conduit. Research into non-invasive vagus nerve stimulation (nVNS) using ultrasound energy has revealed that acoustic stimulation of the vagus nerve can activate the cholinergic anti-inflammatory pathway.
When vagal signaling is enhanced, acetylcholine released at nerve terminals binds to α7 nicotinic receptors on immune cells, suppressing the production of pro-inflammatory cytokines like TNF-α, IL-1β, and IL-6. Studies published in Frontiers in Neuroscience (2024) demonstrate that this pathway also improves mitochondrial function — restoring ATP production, stabilizing membrane potential, and reducing oxidative stress in downstream tissues.
This means ultrasound therapy may not only address local tissue damage but also influence the body's systemic inflammatory tone through neural pathways — a far more comprehensive mechanism than simple heat-and-heal.
What the Clinical Evidence Says
The research landscape for therapeutic ultrasound is broad but nuanced:
- Musculoskeletal pain: Multiple meta-analyses show significant pain reduction in knee disorders, myofascial pain syndrome, and neck/upper back conditions compared to sham treatments. Pulsed ultrasound appears particularly effective for acute pain.
- Fracture healing: LIPUS has the strongest evidence base here, with FDA clearance backed by robust clinical trial data showing accelerated healing timelines.
- Soft tissue repair: Evidence supports improved tendon and muscle healing outcomes, though optimal parameters (intensity, frequency, duration) vary across studies.
- Osteoarthritis: Results are mixed but promising — some studies show increased cartilage thickness and improved joint mobility with consistent treatment.
The American Institute of Ultrasound in Medicine (AIUM) confirms that therapeutic ultrasound at standard clinical parameters shows no adverse biological effects, making it one of the safer options in the physical therapy toolkit.
Practical Considerations
If you're considering ultrasound therapy, here are some factors to discuss with your provider:
- Acute vs. chronic conditions: Pulsed mode is generally preferred for acute injuries (within 72 hours) to avoid exacerbating inflammation through heat. Continuous mode suits chronic conditions where deep tissue relaxation is beneficial.
- Treatment duration: Sessions typically last 5–10 minutes per treatment area. The brevity belies the complexity of what's happening at the cellular level.
- Frequency and intensity: Higher frequencies (3 MHz) target superficial tissues (1–2 cm deep). Lower frequencies (1 MHz) penetrate deeper (3–5 cm). Your therapist will calibrate based on the target tissue depth.
- Combination approaches: Ultrasound therapy is often most effective when combined with exercise, manual therapy, or other modalities that build on the cellular activation it provides.
The Bigger Picture
Therapeutic ultrasound represents something important in modern medicine: a technology that works with the body's existing repair mechanisms rather than overriding them with drugs or invasive procedures. By delivering mechanical energy that cells are biologically programmed to respond to, it activates healing pathways that may have been dormant or insufficient on their own.
As research continues to refine our understanding of mechanotransduction and cellular signaling, the therapeutic applications of ultrasound are likely to expand — from targeted drug delivery through enhanced membrane permeability to precision stimulation of specific neural pathways. The sound wave, it turns out, has a lot more to say than we realized.
References
- Physiopedia. "Therapeutic Ultrasound." Comprehensive overview of mechanisms and clinical applications.
- NCBI StatPearls. "Therapeutic Ultrasound in Physical Therapy." NBK547717
- Defined et al. "Mechanotransduction and therapeutic ultrasound in cellular repair." PMC7563547.
- Watson T. "Ultrasound and cellular repair mechanisms." Physical Therapy 81(7):1351.
- Zhao et al. "Low-intensity pulsed ultrasound for myofascial pain." PMC11337181.
- Khanna et al. "LIPUS and soft tissue repair." PubMed PMID: 30198009.
- ClinicalTrials.gov. "Wearable ultrasound for trapezius pain." NCT02135094.
- Liang et al. "Ultrasound for musculoskeletal pain: systematic review." PMC11664893.
- Frontiers in Neuroscience (2024). "Vagus nerve stimulation and cholinergic anti-inflammatory pathway." doi: 10.3389/fnins.2024.1490300
- AIUM. "Statement on Biological Effects of Therapeutic Ultrasound."